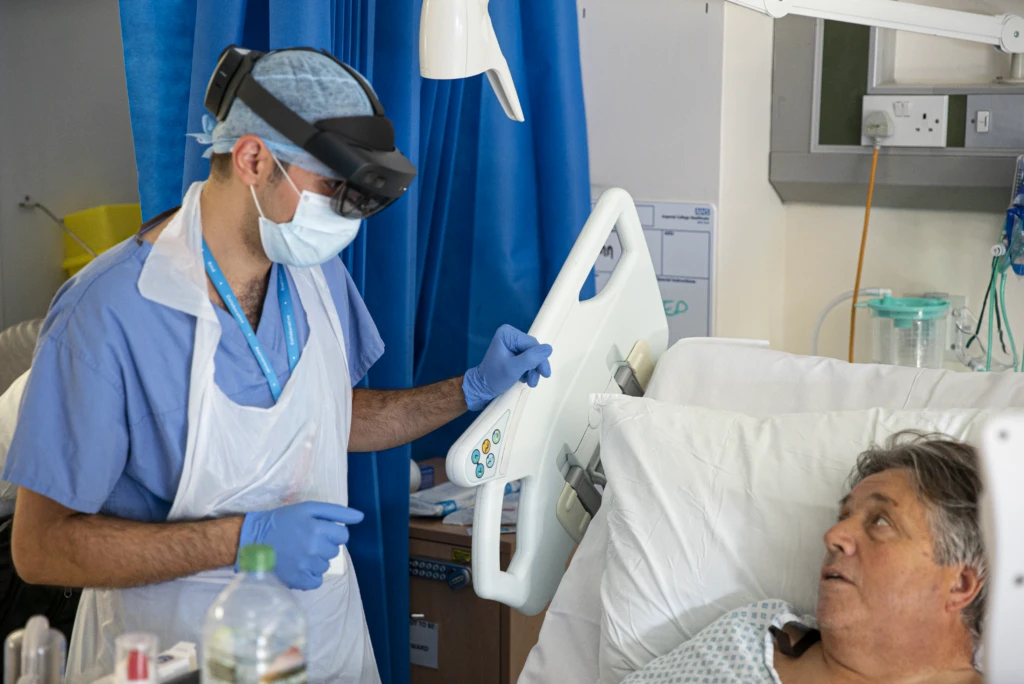
Defining and implementing HoloLens and Dynamics 365 Remote Assist use cases
![]() This is a part of a series of posts about how the HoloLens and Dynamics 365 Remote Assist helps the NHS provide patient care. See the other blog posts here.
This is a part of a series of posts about how the HoloLens and Dynamics 365 Remote Assist helps the NHS provide patient care. See the other blog posts here.
Starting from the beginning of March, we’ve learned a tremendous amount around the use of the HoloLens 2. We now want to use this to help inform our journey as we move forward with more NHS Trusts and more use cases.
Defining the objectives for the remote assist use case
The healthcare service faces unprecedented challenge when necessities such as physical contact with patients, close teamwork, and regular face-to-face communication suddenly become a luxury.
One of our partners, Imperial College Healthcare NHS Trust defined their objectives as:
“The overriding priority for Imperial was to utilise the technology to improve staff safety, and as a secondary output reduce PPE use. This needed to be achieved whilst at least maintaining the same quality of care for patients. The individual use cases then were found based on team structures and staff who were keen to participate and drive the project forward.”
Guy Martin, Department of Surgery and Cancer, Imperial College Healthcare NHS Trust
 On the other side of the country at Alder Hey Children’s Hospital, Rafael Guerrero and his team look after children with congenital heart disease in the North West of England, Cumbria, and North Wales. “We have to quickly adopt the HoloLens 2 and the Remote Assist platform to help our local specialists look after these sick children when they are waiting for the operation,” Guerrero said. “The parents need to be assured that the care of their children is not compromised, and to do this, we need good technology that is proven to work.”
On the other side of the country at Alder Hey Children’s Hospital, Rafael Guerrero and his team look after children with congenital heart disease in the North West of England, Cumbria, and North Wales. “We have to quickly adopt the HoloLens 2 and the Remote Assist platform to help our local specialists look after these sick children when they are waiting for the operation,” Guerrero said. “The parents need to be assured that the care of their children is not compromised, and to do this, we need good technology that is proven to work.”
Process for choosing wards and use cases
Patient care and staff safety
Imperial’s objective was to create “entirely virtual ward rounds”, using the HoloLens 2 as a way to share information and communicate more effectively “at the bedside”.
The first ward the team focussed on was the COVID-19 ward. It was flooded with patients and general medical teams would have high exposure rates. A classic ward round would include a consultant physician, with two or three juniors plus nurses. That makes a potential seven or eight frontline NHS staff exposed with each patient.
In the second ward, the team focused on an area delivering specialist invasive respiratory support. Experts are often distributed throughout the hospital so that the value of bringing in an expert into the bedside virtually is invaluable. In addition, the aerosol generating procedures utilised whilst providing respiratory support placed staff at a much higher risk of infection.
These two examples were also adopted at the Heart Centre at Alder Hey. The number of staff contact per patient during the ward round was five or seven. This was reduced to just one or two with the use of the HoloLens 2 with Dynamics 365 Remote Assist.
St. Mary’s within Imperial Healthcare NHS Trust, is also a major trauma centre, so that was another key area, alongside the surgery department. The ability for quick remote collaboration with an expert from any discipline, can have major benefits. Not only was the interpretation of the main operator communicated to the external experts, but the entire team can share direct visuals of the problem. This saves time and improves the accuracy.
Cardiac unit doctors and nurses promptly adopted this unique communication platform. This helped to deliver care at the same standard as it was before social distancing was enforced. Expert care, efficiency, or staff safety were not compromised by the physical barrier imposed by infection control.
Each of the four use cases were up and running by the end of March and in consistent use with results covered.
Remote expert advice

Morecambe Bay are a group of small, district general hospitals with limited staffing in a semi-rural area. Because of this, their use cases are focused on using Dynamics 365 Remote Assist to train middle-level clinicians such as Specialist Registrars and clinical nurse specialists. They can then make Teams calls to their on-call Respiratory Consultant Physician, who may be in a different part of the hospital, or on call overnight at home, or in a different hospital in the region. This allows them to take the bedside and patient, wherever they are, and support assessments and appropriate treatment plans, including where necessary, rapid escalations of care.
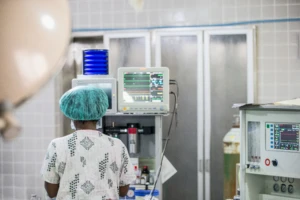
The Alder Hey Heart team has also carried out a pilot supporting non-expert echocardiographers (middle grade cardiology trainees, or paediatricians with interest, or non-paediatric echocardiocardiographers) to perform complex ultrasound scans of children’s hearts remotely. Cardiologist Dr Phuoc Duong has articulated that there was “perfect vision” of the echo machine screen and the ability to guide the non-expert operator in real-time. These are also perceived as excellent training opportunities for novices. They are aiming to run a follow-up study on the benefit of training once the pandemic is downgraded.
Clinical education
Like many teaching hospitals in the country, the Imperial College NHS Trust team undertakes vital training roles to future undergraduate and postgraduate doctors. Virtual training rounds have now started to be implemented with positive initial feedback.
For Leeds Teaching Hospital Trust:
“Our aim is to explore new technologies to improve medical education. We have partnered with the Microsoft lead ResilientXR consortium alongside Health Education England to build COVID-19 content. In addition, we see a significant opportunity to train the next generation of medical students and have developed a core team of trainees and fourth year medical students to explore mixed reality use cases across the hospital including applications in oncology, intensive care, surgery, and also engage with colleagues in the community”
Andrew Lewington, Associate Medical Director of Education, Leeds Teaching Hospital Trust
What were keys to successful implementation?
James Kinross and Rafael Guerrero both shared that in the beginning, there was a fair degree of anxiety. To actually try to deploy new technology in the middle of a storm is hard to do. There’s less resources and less in-person IT support. You’re asking your frontline care workers to do technically difficult things while they’re cognitively over-burdened and stressed and sometimes can’t conceptualise what new technologies can do.
To this end, there are key tips that are worth calling out:
- It’s critical that when the doctor or nurse puts on the HoloLens and makes their first call, it’s ready to go, including compliance, security, and manageability.
- One of the first things that the NHS teams did, were to ensure that HoloLens could work effectively with various different types of PPE – including full face masks. They were able to do this pretty easily with some low-tech solutions. Imperial are planning for longer-term solutions with 3D printed additions.
- Cleaning of HoloLens was also very straightforward within the NHS as they have many protocols for how equipment and devices get cleaned. The NHS found that through collaborating within the consortium, they were also able to leverage best practices very quickly.
- And finally, from a data governance perspective, it was important that patient privacy was adhered to. This included ensuring that clinicians wearing the HoloLens are always identifying what HoloLens is, why they are wearing it, and what the other healthcare workers on the end of the Teams call can see and hear. There were also decisions about what data they would and would not record, in adherence with internal data governance policies.
Identifying and supporting end-user adoption
In the case of Morecambe Bay, CCIO Colin Brown spent a fair bit of time in the first few weeks engaging across the physical NHS Trust locations to meet with Respiratory Consultants, Specialist Registrars, Clinical Nurse Specialists, and Ward Nurse Managers to secure their interest, engagement, and adoption.
At Alder Hey Children’s Hospital, Rafael Guerrero showcased his examples starting from the Heart Centre, with quality improvement survey results to the hospital executive boards. He then subsequently expanded to meetings with heads of departments and education partners from the local universities.
From the Imperial perspective, they also met with many different physicians across Imperial. They showcased the technology to see if there was an immediate use case. If not, they didn’t try to force it. However, what they found is that as teams have more bandwidth or have experienced HoloLens on the Teams-side of the call, they are seeing significantly more requests by others to adopt this technology for remote collaboration.
Getting the foundational use case right
By starting with remote assist, HoloLens is being seen as a functional tool to support remote collaboration and it is adopted on this basis. However, it only taps into a limited amount of the HoloLens functionality. Clinicians are asking for more capability, such as integrating Electronic Health Records. These requests are being easily solved without significant development resources.
Find out more
How HoloLens and Dynamics 365 Remote Assist helps the NHS provide patient care
Measuring patient and clinical effectiveness
What’s next: How can other NHS Trusts get involved?
What technology was needed to get started
About the author
 Leila has been working on the commercial mixed reality business for the last five years and is based in the UK. She’s been working with some of the most advanced customers and partners in the world, helping them identify, pilot and deploy technologies that have a profound ability to transform their business.
Leila has been working on the commercial mixed reality business for the last five years and is based in the UK. She’s been working with some of the most advanced customers and partners in the world, helping them identify, pilot and deploy technologies that have a profound ability to transform their business.
Prior to joining the mixed reality team, she held several senior positions at Microsoft including leading consumer and commercial business units such as Server & Tools and Windows in the UK and Central & Eastern Europe




