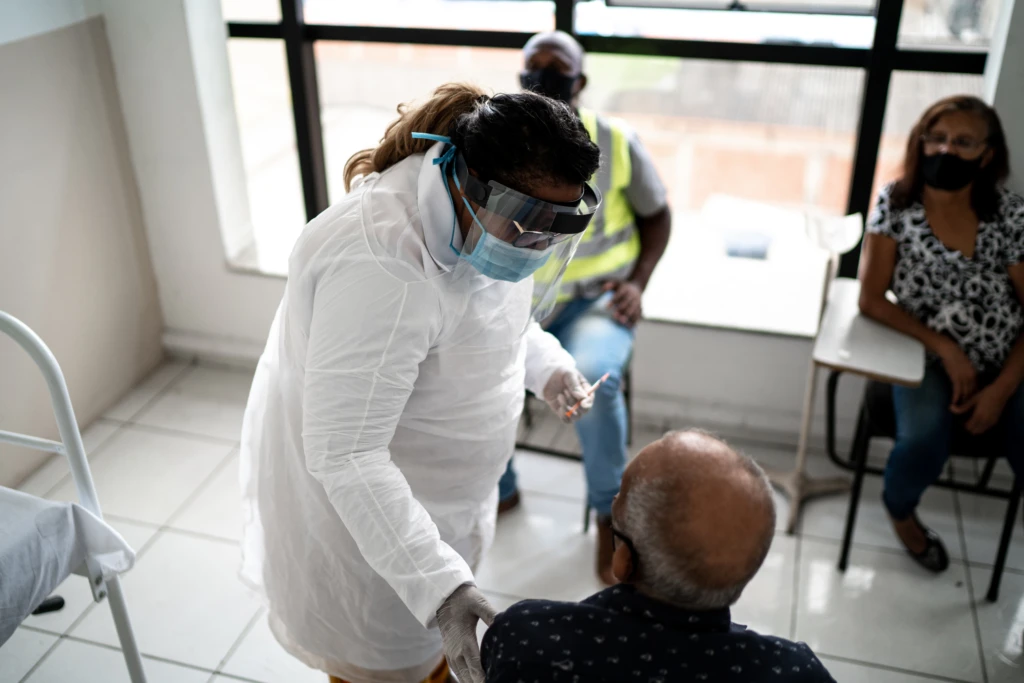
Developing public-private partnerships to address health inequities
Health and vaccine inequities
The pandemic has exposed long-standing inequalities in healthcare and created a stark contrast between the haves and have-nots. At the country-level, developing countries still do not have enough COVID-19 vaccine to cover the majority of its population. Within developed countries and specifically in underserved communities, vaccine hesitancy remains high and COVID-19 vaccination rates remain low. While several factors contribute to vaccine hesitancy, such as awareness and education, perhaps one of the more difficult ones to overcome is the deep and long-standing distrust of government, public health, and the scientific community that many in underserved areas share.
Vaccination equity initiative
Microsoft and its partners have implemented technology platforms globally to enable the scheduling, registration, and data management for COVID-19 vaccinations and have observed first-hand that community-led, public-private partnerships can be effective in addressing vaccine hesitancy and in improving vaccination rates in underserved areas.1-3 In an effort to share what we have learned, we launched the Vaccination Equity Initiative (VEI) in February 2021. Leveraging the momentum of providing COVID-19 vaccines, VEI has been initially focused on COVID-19 vaccinations while also expanding to other critical vaccines/conditions to improve overall health and build more resilient communities.
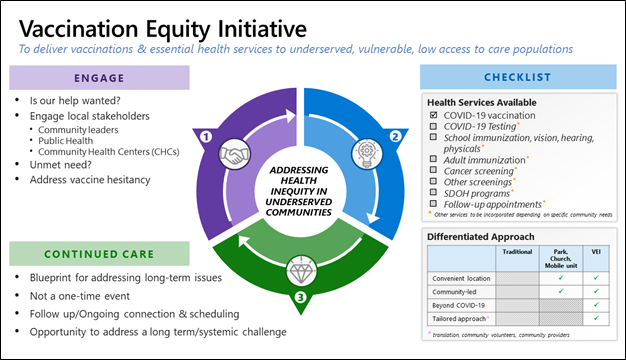
The objective now is to deploy a similar approach across the nation and world. To do this, a coalition of non-profits (e.g. Easterseals, American Heart Association, California Health Medical Reserve Corp [CH MRC]), healthcare organizations, technology enablers (e.g. Microsoft, Accenture) and other key stakeholders are collaborating with local public health, community-faith-based organizations, and other groups to implement these strategies, share their “best practices,” distribute their operations playbook, and provide services and technologies as needed to deploy pop-up vaccination sites in underserved areas.
The goal is to deliver vaccinations and essential health services to underserved, vulnerable, low access to care populations. For additional information about the Vaccination Equity Initiative, please contact VEI@Microsoft.com.
The following blog describes (1) when VEI is most relevant, (2) the simple steps needed to apply VEI, (3) results we’ve seen, and (4) how organizations can learn more about VEI.
Major phases of vaccination deployment
As the pandemic has progressed and vaccination rates have increased, we have observed four (4) phases of vaccination deployment.
- Phase 1. Prioritization, volume, and speed. In this phase, vaccinations were provided by appointment only to eligible healthcare providers and high-risk individuals at mass vaccination sites, hospitals, and retail clinics. The goal was to enable vaccinations for as many persons as possible, as quickly as possible, and in a prioritized manner. Phase 1 also included a nationally coordinated program to vaccinate nursing home residents and staff.
- Phase 2. Accessibility and convenience. This second phase, which commenced sometime during Phase 1, focused on making vaccinations more accessible for the vulnerable and underserved populations. This involved setting up pop-up clinics and deploying mobile vaccination vans and buses in parking lots, schools, churches, parks, and other convenient neighborhood locations. Walk-in appointments were permitted.
- Phase 3. Hesitancy. The third phase involves addressing vaccine hesitancy. Hesitancy is often a result of concerns or fears that individuals may have regarding the vaccine, its potential side effects, and/or how the vaccine was developed. Disinformation, mistrust of the government, and concerns over infringement of civil liberties can also lead to vaccine hesitancy.
- Phase 4. Return to work, school, travel, and events. The pandemic has taken a serious toll on our physical and mental health, economy, education, work life, and personal life. Our ability to restore these essential elements of personal, work, and community life requires that we diminish the amount of virus circulating in the community and enhance our ability to defend against the virus, both physically (e.g., through masks, social distancing, air circulation,) and immunologically (e.g., through vaccinations). As we look forward to a safer return to work, school, and travel, the following strategies help us mitigate risk and provide reassurance:
- Self-attestation: to acknowledge that one does not have symptoms consistent with COVID-19 or recent exposure to individuals infected with COVID-19
- Testing: to demonstrate a negative COVID-19 test result
- Masking: to prevent the spread of infection
- Verifiable credentials: to show verifiable documentation of COVID-19 vaccination and/or a negative test result
- Booster shots: booster shots can help address the emergence and rapid spread of the more elusive and lethal variants by enhancing one’s immunologic response to the variants. Booster shots are particularly important for individuals with immunosuppression, chronic conditions, and advanced age.
Collectively, our goal is to advance as quickly as possible to Phase 4. However, it is difficult, if not impossible, to enable a safer return to work, school, and travel without adequately addressing Phase 3, vaccine hesitancy. The good news is that we now have a much better understanding of how to overcome vaccine hesitancy.
Vaccine hesitancy
In working with local community leaders, we have learned that vaccine hesitancy, specifically in underserved communities, can be addressed when local communities follow these fundamental steps:
- Community Engagement. These initiatives require input, guidance, and active support and engagement from local community leaders and nonprofits who understand the culture, challenges, and best ways to engage members of the community. Other key stakeholders include county +/- state public health agencies and local healthcare providers. Technology enablers can support these efforts through pop-up vaccination management systems for those without Electronic Health Record Systems (EHRs) and ensure that clinical data flows seamlessly and securely between such systems and state immunization registries.
- Family Events. Many individuals who are vaccine hesitant will not attend a COVID-related vaccination event. However, they will attend a community fair, celebration of a holiday, or an event to help bring the kids back to school. The goal is to combine a high interest community based non-COVID-19 focused event (preferably one that is already being planned) with a health fair that includes COVID-19 vaccinations and much more. The event needs to be open to the entire family and ideally should offer fun and entertaining activities for kids.
- Unpressured Conversations. Conversations with those who are hesitant should be unpressured and delivered by individuals who have a long-standing trusted relationship with the community and/or have a healthcare background that allows them to address the specific COVID-19 questions and concerns.
- Volunteers. Key activities that volunteers can assist with include:
- Parking, crowd, and line management
- Translation services
- Registration and scheduling
- Monitoring post-vaccination
- One of the more important roles for the guide is to physically walk interested persons to the vaccination areas
- Vaccination and other essential health services. Consider offering the following health services at the event:
- COVID-19 vaccination and testing
- School immunizations, vision, hearing, physicals
- Adult immunizations
- Cancer screenings
- Other screenings (e.g., hypertension, diabetes, prenatal, high-risk sexual [including testing for sexually transmitted diseases], substance abuse, violence)
- Social Determinants of Health (SDOH) programs (e.g., health insurance. food insecurity, transportation, housing, job, childcare, health education, skills training)
- Address registration barriers. Key challenges may include:
- Language barriers, literacy, and health literacy
- Concerns about deportation
- Concerns about cost
- Lack of health insurance
- Lack of a healthcare provider
- No computer access
- No cell phone access
- Follow-up. It would be helpful for a volunteer to contact high-risk individuals (e.g., homeless, elders living alone, individuals struggling with mental health issues or substance abuse) to ensure that they are able to attend the follow-up appointment(s). Volunteers should be empowered with resources to address communication, transportation, and/or scheduling issues.
Results
These best practices have been applied with great success in Washington, California, Georgia, and other parts of the country.
In the Seattle area, vaccination efforts coordinated by Microsoft, EvergreenHealth, Overlake Medical Center & Clinics, and Public Health – Seattle and King County have delivered to-date over 170,000 vaccinations. Fifty-three percent of doses have been provided to at-risk Black, Indigenous, and People of communities of color.
On May 2, 2021, the VEI King County partnership hosted a pop-up event with Centro Cultural Mexicano featuring Spanish speakers at every corner, cultural works on display, and mariachi music filling the air. Thanks to these efforts, several hundred community members found the access and encouragement they needed to take the first step in the process. Those vaccinated at the event were 98 percent Latino, from 68 zip codes, and 30 cities.
Another key metric for success has been vaccine hesitancy and the percentage of people returning for their second visit. In Central California, where many migrant farm workers reside, vaccination rates have been close to 20 percent. Working in close collaboration with local public health, healthcare, community-based organizations, and local businesses, the California Health Medical Reserve Corps (CH MRC), local public health, community health centers, and Microsoft have hosted several VEI events. We have observed over a 90 percent return rate for the second shot, with a significant increase in the number of people attending the second event as compared to the first event. Many of the first-shot recipients brought their entire families, friends, and neighbors to participate in the second event.
In August and September of 2021, Easterseals, American Heart Association, Emory Health, Accenture, and Microsoft worked in close collaboration with local public health and community leaders who hosted two events that combined “Return to School and Literacy” days with health fair events in Clarkston, GA,. Clarkston is known for its ethnic diversity and has a large refugee population. The events offered activities for the kids and families and provided a variety of health services including COVID-19 shots, childhood immunizations, school physicals, vision tests, and blood pressure screening. Approximately 400 people attended the August event, with 1/3 of them receiving the COVID-19 vaccine. The September event had lower attendance than expected due to the rapid rise in the Delta variant, with many in the community fearing bringing children to large in-person events. 150 families attended where historically this event has 3 – 4 times this attendance. As a result, vaccination rates were lower than the August event however an unexpected ancillary benefit was that the nice weather allowed the children to interact and play with each other—a positive mental health opportunity for children who have been predominantly isolated since the beginning of the pandemic. In addition to adult/vaccine, children services provided a physical exam including screening for height, weight, BMI plus vision and hearing; a significant value-add to this community in addition to the vaccination services provided.
Key success factors have included:
- Focusing on areas with the highest risk and most impacted individuals.
- Working closely with local communities to plan and coordinate events.
- Making registration easy.
- Hosting events during off-hours and weekends at convenient locations.
- Addressing transportation and mobility needs.
- Providing vaccinations regardless of immigration status.
In closing, I’d like to share a few remarks from our VEI Coalition members on why continued work to address vaccine equity is so important and how their organizations’ are contributing to the effort:
“For the health of us all, it’s vital that we address vaccination hesitancy with compassion rather than disdain. We can present the science through trusted medical experts and meet people where they are in their understanding of virology. Vaccine hesitancy doesn’t just come from misinformation, but from historical and current traumas as well – an important consideration as we reach out to communities of color. Beyond hesitancy, we must continue finding ways people with disabilities and the aging community can access vaccines safely, whether it’s receiving the shots at home, or finding transportation to a vaccine center. Easterseals is committed to looking at the whole picture when reaching out to communities, ensuring as many individuals as possible can receive these vaccines.” —Angela Williams, President and CEO of Easterseals.
“As champions for health equity, the American Heart Association recognizes the importance of efforts in the community that bridge gaps between healthcare and the people who need it. Here in Atlanta, we’ve worked tirelessly for decades to improve the health of our residents, and we value this collaboration of like-minded organizations to equitably improve rates of COVID-19 vaccination.“ —Carla Smith, Vice President of Health Strategies for the American Heart Association in Atlanta.
This pandemic has spotlighted the health inequalities that many communities experience every day. Critical components in the system did not have the capacity or the tools to ensure accurate and real time data exchange which slowed down the efforts to get vaccinations to the communities that needed it the most. The work that we are doing to bridge these gaps is rooted in the community-first approach with a lens of equity and inclusion. It is imperative that we engage with the trusted voices within the community to help guide our efforts, which will help address hesitancy as well as get more people vaccinated. Our focus is to have the greatest local impact through data sharing, collaboration and ensuring equity.” —Dr. Greg Buchert, Chief Medical Officer, CHMRC.
References:
- Helping communities accelerate COVID-19 vaccinations at the last mile – Microsoft Industry Blogs
- Secure, safe, and equitable vaccine distribution – Microsoft Industry Blogs
- A Global Focus on Health Equity – HLTH
Learn more about Microsoft for Public Health and Social Services and how the use of technology helps to create opportunities for safety, wellness, and prosperity.




